
What is a Seton Suture? Complete Guide to Anal Fistula Treatment
Hoss Agina
Feb 21, 2026
A seton suture is a surgical thread or rubber material placed through an anal fistula tract to maintain drainage and facilitate healing while preserving anal sphincter function. This minimally invasive procedure serves as both a temporary drainage solution and a staging technique for complex anal fistula treatment.
Seton placement represents one of the most effective approaches for managing anal fistulas that involve significant portions of the anal sphincter muscles, offering superior outcomes compared to immediate surgical closure in complex cases.
TLDR: Key Points About Seton Sutures
- Seton sutures are surgical threads placed through anal fistula tracts to maintain drainage and facilitate healing while preserving sphincter function
- Success rates range from 78-100% with proper patient selection and technique
- Loose setons preserve continence better than cutting approaches, though healing may take longer
- Complex cases involving significant sphincter muscle benefit most from seton-based staging approaches
Master Surgical Skills with Professional Training
Understanding complex surgical procedures like seton placement requires comprehensive knowledge of suture techniques and anatomical principles. Whether you're studying colorectal surgery or general surgical skills, hands-on practice with quality training materials makes the difference between theoretical knowledge and practical competence.
Develop your surgical skills with our All-in-One Suture Practice Kit, designed by chemical engineers to provide realistic practice scenarios that prepare you for real clinical situations. Master the techniques that save lives and improve patient outcomes.
Understanding Anal Fistulas and Why Setons Are Necessary
An anal fistula is an abnormal connection between the anal canal and the skin around the anus, typically developing after an abscess forms and drains. According to the Mayo Clinic, these abnormal connections create persistent drainage, discomfort, and risk of recurring infection.
The fistula tract can involve varying degrees of the anal sphincter muscles, which control bowel movements and maintain continence. When a significant portion of these muscles is affected, direct surgical treatment through simple closure carries high risks of faecal incontinence.
Types of Anal Fistulas
Complex anal fistulas involving substantial sphincter muscle require careful management to balance healing with preservation of bowel control. The Cleveland Clinic classifies fistulas based on their relationship to the sphincter:
- Intersphincteric fistula tract - passes through the internal sphincter only
- Transsphincteric fistula - crosses both internal and external sphincters
- High anal fistulas - involve upper portions of sphincter complex
What is a Seton Suture? Types and Functions
A seton consists of surgical thread or rubber material threaded through the entire fistula tract to maintain an open pathway for drainage. This string like material serves multiple therapeutic functions depending on how it's configured.
Loose Seton
A loose seton maintains the fistula in an open state without applying cutting pressure to surrounding tissues. This approach:
- Provides continuous drainage of infected material
- Prevents abscess reformation
- Allows inflammation to resolve naturally
- Preserves anal sphincter function completely
Research published in Nature Scientific Reports demonstrates that loose seton approaches achieve excellent healing rates while maintaining superior continence outcomes.
Cutting Seton
A cutting seton treatment applies controlled tension to gradually tightened the material, which slowly cut through tissues over time. This cutting seton approach:
- Progressively divides the involved sphincter muscle
- Allows tissue to heal as division occurs
- Achieves faster closure than loose techniques
- Carries higher incontinence risks
Studies show cutting seton treatment can achieve healing in several weeks to months, though patient selection remains critical for optimal outcomes.
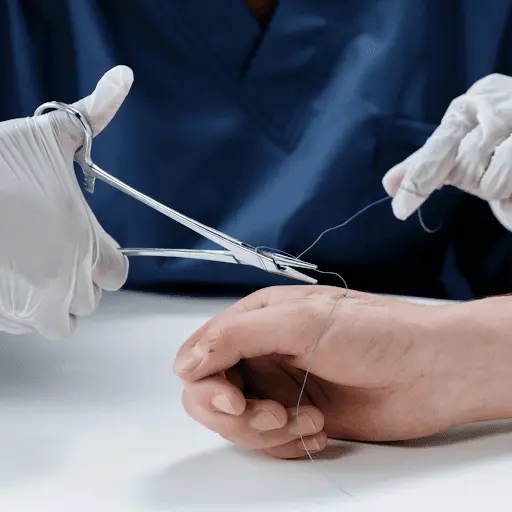
The Seton Procedure: What to Expect
Anal fistula surgery involving seton placement typically occurs under general anaesthetic as an outpatient procedure. The NHS outlines the standard approach:
During Surgery
- Colorectal surgeon locates both internal and external fistula openings
- Fistula passes are carefully mapped using specialized probes
- Seton material is threaded through the complete tract
- Material is secured with appropriate tension based on treatment goals
Recovery Process
Most patients experience mild pain for 1-2 weeks following seton treatment. Bowel movements typically normalize within days, though some adjustments may be necessary.
Sitz baths in warm water help maintain cleanliness and promote comfort during healing. This involves sitting in a shallow bath for 15-20 minutes after bowel movements.
For those interested in learning about surgical techniques and suture materials, exploring a comprehensive suture practice kit can provide valuable hands-on experience with various surgical materials and methods.
Treatment Outcomes and Success Rates
Clinical research demonstrates impressive healing rates with seton-based approaches. A foundational study examining routine seton placement reported:
- 78% complete healing in patients
- 9-week median healing time
- Zero incontinence complications
- Universal patient satisfaction
Comparing Treatment Approaches
Different fistula treatment methods show varying success patterns:
- Seton drainage: 78-100% healing with preserved continence
- Fibrin glue: 14-70% success rates with high recurrence
- Advancement flap: 62-93% success in complex cases
The recurrence rates favor seton approaches, particularly for high anal fistulas where sphincter preservation is paramount.
Special Considerations for Complex Cases
Crohn's Disease and Inflammatory Bowel Disease
Patients with inflammatory bowel disease like Crohn's disease require modified approaches to treat anal fistulas. These conditions create ongoing inflammation that complicates healing, often necessitating long-term seton retention combined with medical therapy.
Perianal Fistula Management
Simple fistulas may heal with basic drainage, while complex cases involving sphincter muscles benefit from staged approaches. The evolution of surgical sutures demonstrates how surgical techniques have evolved to address these challenging cases.
Understanding these advanced surgical concepts can benefit medical students interested in choosing the right suture practice kit for their training needs.
FAQ
Frequently Asked Questions
Dissolvable stitches and absorbable stitches dissolve at different rates depending on the material used. Tissue adhesive and modern synthetic absorbable sutures typically dissolve over 8-16 weeks, while traditional materials like plain catgut dissolve within 7-10 days. The body heals around these materials as they break down naturally, eliminating the need for removal appointments.
Several alternatives exist for close wounds besides traditional stitches or staples. Skin glue (tissue adhesive) works well for small, clean cuts and dissolves naturally. Butterfly bandage strips can hold minor wounds together. Steri strips provide external support similar to tape. Staples offer quick closure for longer surgical incisions. Your doctor will recommend the best option based on wound characteristics and location.
Normal healing properly shows signs of gradual improvement over time. Expect some little redness and swelling initially, which should decrease daily. The wound should remain intact without gaps or separation. Very thin layer of clear drainage is normal initially, but pus or increasing pain indicates problems. About two weeks after surgery, most wounds show significant healing progress.
Different types of stitches have varying removal schedules. Non-absorbable sutures like nylon require manual removal according to anatomical location guidelines. Absorbable stitches dissolve naturally and don't need removal. Called sutures by medical professionals, these materials serve different purposes—some provide temporary support while others offer permanent reinforcement for deep tissue layers.
Getting doctor's approval before resuming normal activities ensures your wound can handle increased stress. Avoid sports and strenuous activities until cleared because tissue needs time stitches to develop adequate strength. Physical activity too early can cause the wound to re open, leading to complications. Your healthcare provider will give specific instructions based on your individual healing process and injury type.
After removing sutures, continue gentle skin care to optimize healing. Apply a thin layer of recommended ointment to keep the area moist. Avoid soaking the wound in water for several few weeks. The covered area should be protected from sun exposure to prevent infection and minimize scarring. Follow up care appointments allow your surgeon to monitor progress and address concerns during the body heals completely over the following weeks.
